Peptic Ulcer
By Dr. Kenneth Wang
Peptic ulcer disease (PUD) is a mixed group of disorders that involve the gastrointestinal (GI) tract. The stomach and duodenum (upper part of the intestine) are the most common locations where ulceration occurs. The rate of occurrence of PUD is variable and depends on ulcer type, age, gender and geographic location. For example, in Japan, stomach ulcers occur at five to ten times the rate of duodenal ulcers, while in the United States and most European countries duodenal ulcers are about two times as common as stomach ulcers.
Individuals with chronic peptic ulcer disease will experience periods of remission and recurrence of the disease, while acute peptic ulcers are limited to a specific patient population and clinical scenario. When left untreated, PUD may result in serious complications such as gastrointestinal bleeding and cancer. Stomach ulcers are much more likely to result in death or disability due to a greater likelihood of causing hemorrhage, perforation, or obstruction. In addition, while duodenal ulcers are almost never cancerous, approximately 55% of stomach ulcers are cancerous.Â
Peptic ulcer is a terminology that belongs to modern medicine; there is no mention of it in the history of Traditional Chinese Medicine (TCM). Instead, because of the nature of its symptoms, it is categorized as “stomach ache” or “epigastric pain.” It is associated with the spleen, liver and gall-bladder because these organs play an important role in the development of the disease.Â
According to the five elements theory, the spleen and stomach belong to earth, and the spleen has an interior-exterior relationship with the stomach. Both of these organs are responsible for the digestion, absorption and transportation of food, and control blood production and its circulation.Â
The liver and gall-bladder belong to wood and they jointly regulate qi (vital energy) and the emotions, enhancing digestion and blood flow. In normal circumstances, wood (liver and gall-bladder) restricts the earth (spleen and stomach) which means that the spleen and stomach are under the control of the liver and gall-bladder. If the liver is hyperactive, it unduly restricts functioning of the spleen, causing an imbalance in the body. According to the five elements theory, the resulting situation is described as “wood overacting on earth.”
Causes
According to TCM, peptic ulcer can be caused by any of the following:Â
1. Dietary injury
Diet is an important cause of  stomach disorders. The stomach receives and ripens food; the spleen transforms and transports refined nutrient essence up towards the lungs, whilst the stomach sends waste down towards the intestines. The descending function of the stomach corresponds with the ascending function of the spleen, and this is crucial in ripening, transporting and transforming nutrient essence and wastes in the middle burner. Improper eating habits affect the stomach easily which leads the stomach-qi to flow in the wrong direction, and results in nausea, vomiting, hiccups or belching.
2. Emotional distressÂ
Emotional problems have a profound influence on stomach disorders. When emotions such as anxiety, pensiveness, grief and anger predominate, liver yang ascends and liver qi stagnates which, in turn, affects the functioning of the spleen and stomach. In the absence of the liver’s regulatory function, the spleen cannot successfully transport and transform food into qi and blood, and the stomach cannot send waste down to the intestines. This causes epigastric pain, belching or nausea.
3. Weakness of spleen and stomach
This may be due to genetic constitutional weakness, or mental over-exertion over a long period. A person tends to get digestive problems like a poor appetite, vomiting or diarrhea, and possibly also muscle weakness and low energy. When attacks from pathogenic factors become more serious, stomach disorders occur easily.
Symptoms
Gastric pain, a major manifestation of peptic ulcer, usually occurs in the epigastric region or upper abdomen. Episodes of pain may be periodic, rhythmic or chronic. If seasonal, the pain usually occurs in late autumn, and the nature of pain is manifested as a dull, stabbing, distending, burning or hunger pain. Among the different types of pain, intermittent mild dull pain is most frequent. This usually lasts one or two hours but, in rare cases, it can last several days. The pain can be relieved by alkaline drugs or food. Along with pain, associated symptoms are belching, sour regurgitation, excessive saliva, nausea or vomiting.Â
|
The location of gastrointestinal (GI) ulcer can be implied by the symptoms. People with stomach ulcers usually complain of pain being caused or worsened by food. They also describe the pain as being widespread over the lower abdomen. When someone has a duodenal ulcer the pain is typically described as sharp and burning in nature with a specific point of tenderness. In contrast to stomach ulcers, people with duodenal ulcers usually experience relief of pain with food. Other symptoms of a duodenal ulcer include a feeling of abdominal pressure, fullness or hunger. People with duodenal ulcers may also be awakened at night due to the normal nighttime peak in acid secretion. It is important to be aware of “alarm symptoms” which can be present in people who have serious complications from peptic ulcer disease (PUD) such as bleeding or people with stomach cancer. These “alarm symptoms” include weight loss, vomiting, back pain, vomit that has the appearance of “coffee grounds” and dark tarry stools. |
|
|
Diagnosis
Diagnosis in TCM places importance on determining the circumstances and manifestations of a disease through inquiry and observation of symptoms. A diagnosis is based on the traditional four examination techniques:
| 1. | Questioning The TCM practitioner will establish the medical history of both the patient and his family. |
| 2. | Observation Examination of the physical features of the body, such as the face, tongue, hair, nails, sputum (mucus that is coughed up), and location of pain, all offer clues to the problem. The tongue is a particularly useful indicator of the functioning of the internal organs. |
| 3. | Listening and smelling The smelling of sputum and breath and listening to the sounds produced by the chest offer additional clues to the patient’s health. |
| 4. | Touching Feeling the pulse is a cornerstone of TCM diagnosis and gives the practitioner much information about any bodily imbalance. |
For details, please see article on “What to Expect from a TCM Doctor’s Examination“.Â
TCM practitioners will usually begin with a thorough investigation of the patient’s complaints and categorize the symptoms under special syndrome groups known as “disharmony patterns.” The disharmony patterns are present at different stages of a disorder. The practitioners will look at both the major manifestations, and “disharmony patterns” which are described below:Â
1. Qi stagnation
The patient feels distending pain in the epigastric region, and fullness and oppression in the hypochondrium (the upper lateral sides of the abdomen). These symptoms would worsen with emotional disturbance, and can be relieved by discharge of intestinal gas or belching. The patient tends to sigh, has a poor appetite and experiences oppression in the chest and sour regurgitation. On examination, the tongue is covered by a thin white fur, and the pulse is taut.Â
2. Heat retention
The patient feels a burning pain in the epigastric area. Eating offers no obvious relief; instead, it may even make the symptoms worse. The mouth is dry with a bitter taste. Other symptoms include thirst and a desire for cold drinks, sour regurgitation, irritability, clamoring stomach and constipation. On examination, the tongue is red with yellow fur, and the pulse is taut or rapid.Â
3. Yin deficiency
The patient feels a dull, burning epigastric pain which becomes worse on an empty stomach. Other associated symptoms include thirst and a disinclination to drink, dryness of the mouth, poor appetite, retching, constipation, and a feverish sensation in the palms, soles and chest. On examination, the tongue is red and dry, with cracks in the central portion. It is covered with little or scattered, cracked fur. The pulse is thready or rapid.
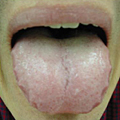 |
| A pale tongue with indented margin, the cracks in the central portion indicate spleen and stomach dysfunction. |
4. Deficient cold
The patient feels a dull epigastric pain which tends to ease with warmth and massage. An attack can be easily induced or worsened by over-exertion. The pain worsens on an empty stomach. Although the pain can be relieved by eating, abdominal distention will follow. Other associated symptoms are fatigue, sleepy, reluctance to speak, and loose stools. On examination, the tongue is pale and bulky with indented margin, and it is covered by a thin white fur. The pulse is deep, thready or slow.
5. Blood stasisÂ
The patient experiences a fixed, stabbing pain in the epigastric area. But when the pain becomes extreme, it sometimes radiates towards the chest and the back. This may be accompanied by coldness of the limbs, sweating, vomitting blood or blood in the stools. On examination, the tongue is dark purple, and may have bruises or patches on the surface. The pulse is hesitant.
In general, during the pathological course of peptic ulcer, the above syndromes develop at different stages. In the early or active stages of peptic ulcer, qi stagnation and heat retention syndromes are quite common. TCM terms these as a sthenia or excess (shi) syndromes in which the body offers a relatively strong resistance.Â
In the late or recovery stages of peptic ulcer, yin deficiency and deficient cold syndromes are more common. TCM terms these as a sthenia or deficiency (xu) syndromes in which the body’s resistance is very weak.Â
Blood stasis syndromes can develop at any stage, but occurs mostly in the middle and late stages. The syndrome has a deficiency nature but presents excitatory signs, or having both excess and deficiency syndromes inter-mixed.
Treatment
In TCM, treatment for peptic ulcer is based on “disharmony patterns,” or therapies according to the western symptoms of peptic ulcer syndromes. An alternative is to integrate western and Chinese approaches to create a synergetic effect on the disease, thus enhancing clinical efficacy. The following are brief introductions to TCM approaches:
| A. Treatment based on TCM syndromes |
Qi stagnationÂ
Therapeutic aim: Soothing the liver to regulate qi. Commonly used prescriptions are modified chaihu shugan tang, sini sanand xiaoyau san.
Sample of Prescription:Â chaihu shugan tang
| chai hu | Chinese tororwax root |
| chen pi | dried tangerine peel |
| shao yao | peony |
| zhi ke | bitter orange |
| zhi gan cao | liquorice root (processed with honey) |
| chuan xiong | Szechuan lovage |
| xiang fu | nut grass |
Heat retention
Therapeutic aim: Soothing the liver and eliminating heat. Commonly used prescriptions are modified huagan jian, zuojin wan and banxia xiexin tang.
Sample of prescription: banxia xiexin tang
| ban xia | pinella tuber |
| huang qin | baical skullcap |
| gan jiang | fried ginger |
| ren shen | ginseng |
| zhi gan cao | liquorice root (processed with honey) |
| huang lian | golden thread |
| da zao | common jujube fruit |
Yin deficiency
Therapeutic aim:Â Nourishing yin to strengthen the stomach. Commonly used prescriptions are modifiedÂ
yiguan jian, yangwei tang and liuwei dihuang tang.
Sample of Prescription:Â yiguan jian
| sha seng | adenophora |
| mai dong | dwarf Lily-turf |
| dang gui | Chinese angelica root |
| sheng di | dried rehmannia root |
| qi zi | Chinese wolfberry fruit |
| chuan lian zi | toosendan fruit |
Deficient cold
Therapeutic aim: Warming the middle burner to strengthen the spleen. Commonly used prescriptions are modified huangqi jianzhong tang, sijun zi tang, lizhong tang and liangfu wan.
Sample of Prescription:Â huangqi jianzhong tang
| huang qi | Mongolian milkvetch root |
| gui zhi | cassia twig |
| zhi gan cao | liquorice root (processed with honey) |
| da zao | common jujube fruit |
| shao yao | peony |
| sheng jiang | fresh ginger |
| yi tang | maltose |
Blood stasis
Therapeutic aim: Activating blood to resolve stagnation. Commonly used prescriptions are xuefu zhuyu tang and gexia zhuyu tang.
Sample of Prescription:Â xuefu zhuyu tang
| dang gui | Chinese angelica root |
| sheng di | dried rehmannia root |
| tao ren | peach seed |
| hong hua | safflower flower |
| zhi ke | bitter orange |
| chi zhao | common peony root |
| niu xi | twotooth achyranthes root |
| jie geng | balloonflower root |
| chuan xiong | Szechuan lovage |
| chai hu | Chinese tororwax root |
| gan cao | liquorice root |
During the treatment, herbs like liquorice root (gan cao), tendrilleaf fritillary bulb (chuan bei), common bletilla tuber(bai ji), notoginseng (san qi) rhubarb (da huang) are added in the prescription for additional relief of dyspeptic symptoms. Some prescriptions to astringe (lessen) acid secretion are effective for related complaints, e.g. mixed powder of thunberg fritillary bulb(zhe bei mu) and cuttle-fish bone (wu zei gu) can be used.Â
| B. Single Proven Prescription |
In practice, a lot of recipes have been proved effective against the disease but were not listed in medical journals. These recipes do not follow any particular diagnostic rules in TCM but are used only when the disease is confirmed as peptic ulcer. For example pearl powder is effective in providing relief from symptoms and speeding up the healing of an ulcer.Â
| C. Acupuncture and moxibustion |
This method is used to provide pain relief, and commonly applied according to the differentiation of the affected meridian. For example, in the case of liver and stomach disharmony, acu-points in the Leg Yang Ming Stomach Meridian and Leg Jue Yin Liver Meridian are chosen.Â

